That quiet tiredness nobody can explain
It starts so gradually you barely clock it. You’re tired — but then, everyone’s tired, aren’t they? You put it down to work, to the kids, to another rubbish night’s sleep. You drink more coffee. You push through. And somewhere around mid-afternoon — say, 3pm on a grey Tuesday — you notice your eyes struggling to focus on the screen, a heaviness settling behind them that no amount of blinking shifts. Your legs ache faintly when you take the stairs, not in a “just done a workout” way, but in a dull, deep way that doesn’t quite make sense.
These are vitamin D deficiency signs, and if you’re living in the UK, there’s a decent chance you’ve felt some version of this without connecting the dots. I certainly didn’t. Not for a long time.
The trouble is, low vitamin D doesn’t announce itself the way a cold does, or a dodgy knee. It creeps. It accumulates. And because the symptoms overlap with about forty other things — stress, poor sleep, ageing, just life — most of us brush it off. Which is precisely why it’s worth paying attention.
What vitamin D actually does (and what happens when you don’t get enough)
Here’s the bit that surprised me when I finally looked into it properly. Vitamin D isn’t really a vitamin in the traditional sense — it’s closer to a hormone. Your body produces it when sunlight hits your skin, and it’s involved in far more than just bones, though bones are where most people’s knowledge stops.
It helps regulate calcium and phosphate absorption, supports your immune system, influences muscle function, and appears to play a role in mood regulation. When levels drop too low, your body starts quietly struggling with all of these at once.
What I’ve noticed, again and again — in friends, family, colleagues — is that people tend to normalise the symptoms. They’ll mention being exhausted or getting every cold going around the office, and when you suggest it might be worth checking their vitamin D, they look at you like you’ve suggested aromatherapy. There’s this assumption that vitamin D deficiency is something that happens to other people. Elderly people. People who never go outside.
It’s not. Current NHS estimates suggest that around one in five adults in the UK has low vitamin D levels. Some researchers think the real figure is higher, particularly during the winter months when we’re essentially running on whatever we stored up during the seven decent days of summer we got.
Common vitamin D deficiency symptoms to watch for:
- Persistent fatigue that sleep doesn’t fix
- Frequent colds and infections — your immune system needs vitamin D to function properly
- Bone and lower back pain — particularly a deep, aching quality
- Muscle weakness or cramps — sometimes mistaken for general unfitness
- Low mood or feeling flat — especially through autumn and winter
- Slow wound healing — cuts and grazes taking longer than they should
- Hair thinning — though this one has many possible causes
Not everyone gets all of these. But most people with genuinely low levels will recognise at least two or three.
What people get wrong about vitamin D deficiency
There’s a lot of well-meaning but slightly misleading information floating around, and — this still irritates me, honestly — much of it comes from the wellness corner of the internet where everything is either a miracle cure or a hidden epidemic.
The first misconception: that you can get enough vitamin D from food alone. You can’t. Or rather, you can in theory, but you’d need to eat oily fish almost daily, consume significant amounts of egg yolks, and probably drink fortified milk like it was going out of fashion. The reality is that food contributes a relatively small amount of your total vitamin D. Sunlight is the main source, and supplementation fills the gap for most people in the UK.
The second: that spending time near a window counts. It doesn’t. Glass blocks the UVB rays your skin needs. That conservatory you sit in on Sunday mornings? Lovely for reading the papers. Useless for vitamin D.
The third, and this is the one that catches people out: assuming that because you “feel fine,” your levels are fine too. Vitamin D deficiency can be subclinical for months or even years. You adapt. You recalibrate what “normal” feels like. You forget what it’s like to not feel slightly run down.
I suppose what I’m trying to say is that the signs of vitamin D deficiency are easy to miss precisely because they mimic the background noise of modern life. Tiredness. Aches. Getting ill a lot. Who doesn’t experience those?
Why living in the UK makes this worse
Let’s be honest about something: we live on an island where meaningful sunlight is seasonal at best. From roughly October to March, the sun sits too low in the sky for UVB rays to penetrate the atmosphere at a useful angle. That’s half the year. In Scotland and northern England, the window is even narrower.
Then there’s the way we live. Office jobs. Commuting in the dark. Weekends spent catching up on housework or shopping. Even in summer, we’re not exactly a nation that spends hours outdoors bare-armed. And when we do get a sunny day, half of us — quite rightly — reach for the SPF 50 because we’ve been told about skin cancer since we were children. Which is important. But it does further reduce vitamin D synthesis.
There’s also that particularly British reluctance to go to the GP about something as vague as “I’m just really tired.” You know the one. Where you rehearse what you’ll say in the waiting room, then feel faintly ridiculous when you’re actually sitting there, and end up saying “It’s probably nothing” before the doctor’s even asked what’s wrong. So you don’t go. You wait. You have another coffee.
The NHS recommends that everyone in the UK consider taking a vitamin D supplement during autumn and winter. People at higher risk — those with darker skin, people who cover most of their skin outdoors, those who spend very little time outside — are advised to consider supplementation year-round. This isn’t fringe advice. It’s on the NHS website. And yet a surprising number of people I’ve spoken to either don’t know this or assume it doesn’t apply to them.
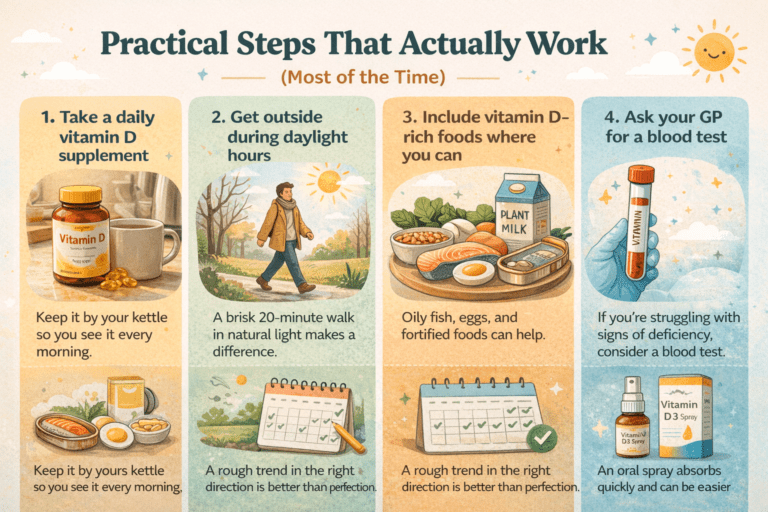
Practical steps that actually work (most of the time)
I realise this sounds like standard advice. Stay with me — because the gap between what’s recommended and what people actually do is where most of us live, and it’s worth being honest about that.
Take a daily vitamin D supplement
The NHS recommends 10 micrograms (400 IU) of vitamin D daily for adults during autumn and winter. Many GPs and nutritionists suggest that people with confirmed low levels may benefit from a higher dose temporarily, but that’s worth discussing with your doctor rather than self-prescribing.
In theory, you’d take it every day without fail. In practice, you buy a bottle, take it religiously for a fortnight, then forget about it until you find the bottle again in April. What actually helps: keeping it next to your kettle, or wherever you make your morning tea. You’ll see it. You’ll take it. It’s not glamorous, but it works better than good intentions.
Vitamin D3 (cholecalciferol) is generally considered the more effective form over D2. Most decent supplements from Boots or Holland & Barrett will be D3. They don’t need to be expensive — the supermarket own-brand versions are usually fine.
Get outside during daylight hours
Even on overcast days, there’s more UVB exposure outside than in. A twenty-minute walk at lunchtime, face and forearms uncovered when the weather allows, makes a genuine difference during the months when it’s actually possible.
Between October and March, this is less about vitamin D production and more about all the other benefits: movement, daylight exposure for your circadian rhythm, fresh air, a brief escape from your desk or kitchen table. Still worth doing. Just don’t expect it to fix your vitamin D levels in January.
Include vitamin D–rich foods where you can
Oily fish — salmon, mackerel, sardines. Eggs. Fortified cereals and some fortified plant milks. Red meat in smaller amounts.
Will this single-handedly solve a deficiency? No. But it contributes, and these are generally decent foods to be eating anyway. If you’re vegetarian or vegan, the food sources are more limited, which makes supplementation even more relevant.
Ask your GP for a blood test
If you’re experiencing several vitamin D deficiency symptoms — persistent fatigue, bone pain, frequent infections, low mood — it’s worth requesting a 25-hydroxyvitamin D blood test. Some GPs will do this readily; others may need a bit of convincing. You might need to be specific about why you’re asking.
The test itself is straightforward. A small blood draw. Results usually come back within a week or two, depending on your surgery. If your levels are significantly low, your GP may prescribe a higher-dose supplement for a few months to bring them up.
Be consistent, not perfect
This applies to supplementation, diet, outdoor time — all of it. You’ll miss days. You’ll eat nothing but toast for a week. You’ll spend an entire Saturday indoors because it’s bucketing down and you simply can’t face it. That’s fine. The goal is a rough trend in the right direction, not perfection.
Consider a vitamin D spray or drops if tablets feel like a chore
Some people genuinely forget tablets or find them annoying to take. Oral sprays (like BetterYou, which is a UK brand) absorb through the lining of your mouth. Some people find them easier to stick with. It’s a small thing, but adherence matters more than format.
When to actually see your GP
I’ll be honest — I ignored my own tiredness and aching legs for about three years before anyone suggested checking my vitamin D. By the time I had a blood test, my levels were properly low. Not dangerously so, but low enough that my GP put me on a loading dose for twelve weeks. Looking back, it’s obvious. At the time, I genuinely thought I was just getting older.
So. Consider booking that appointment if you’re experiencing:
- Fatigue that doesn’t improve with rest, lasting more than a few weeks
- Bone pain that has no clear cause — particularly in your back, legs, or ribs
- Muscle weakness affecting your daily activities
- Noticeably increased frequency of infections
- Significant mood changes, especially seasonal patterns
- Any symptoms in children — bone pain, irritability, delayed growth
If you’re pregnant, breastfeeding, or have a condition affecting nutrient absorption (coeliac disease, Crohn’s, for example), your GP should be aware and may monitor your levels more closely.
Don’t wait until you feel dreadful. That particular British instinct to “not make a fuss” has a cost, and this is one area where catching it early makes the whole thing simpler to sort out.
The quiet, unsexy truth
The quiet, unsexy truth
I’m aware that I’ve just written close to two thousand words essentially telling you to take a vitamin and go outside. It’s not groundbreaking. It won’t trend on social media. There’s no dramatic before-and-after.
But vitamin D deficiency signs are genuinely easy to miss, and the consequences of ignoring them for years — weakened bones, a struggling immune system, a mood that never quite lifts — are real and measurable. The fix, for most people, is cheap, straightforward, and available without a prescription.
I don’t know if this will be the thing that makes a difference for you specifically. Bodies are complicated. Tiredness has a hundred causes. But if you’ve been feeling quietly rubbish for a while and can’t quite put your finger on why, this is one of the simplest things to check and one of the easiest to address.
It might not be the answer. But it might be part of it. And sometimes that’s enough.
This article is for general information and does not replace medical advice. If you’re concerned about your vitamin D levels or any symptoms, please speak to your GP or contact NHS 111.