Is Muscle More Vital Than Your Heart? The New Science
For decades, conventional thinking relegated muscles to a mechanical role: they contract, they relax, and they move bones. That paradigm is now obsolete.
Skeletal muscle comprises approximately 40% of total body mass and functions as the largest metabolic organ in the human body. Research published through the National Institutes of Health confirms that muscle tissue actively participates in whole-body homeostasis through complex biochemical signaling.
The discovery of myokines—hormone-like proteins secreted by muscle fibers during contraction—fundamentally altered our understanding. These molecules communicate with the brain, liver, pancreas, fat tissue, and immune cells. When muscles contract, they don’t just burn calories; they broadcast chemical messages that regulate systemic health.
This positions skeletal muscle alongside the liver, pancreas, and thyroid as an endocrine organ with far-reaching physiological influence.
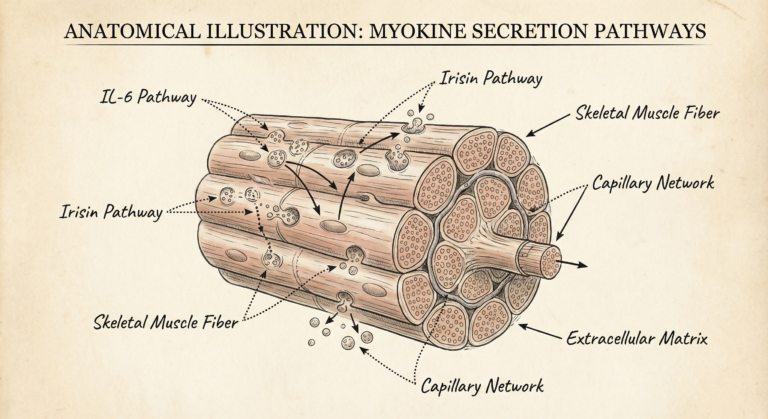
How Muscle Mass Regulates Metabolism
The metabolic implications of viewing muscles as a vital organ are profound. Skeletal muscle serves as the primary site for glucose disposal—meaning your muscles determine how efficiently your body handles blood sugar.
Key metabolic functions include:
- Glucose uptake: Muscles absorb approximately 80% of insulin-stimulated glucose from the bloodstream
- Glycogen storage: Muscle tissue stores carbohydrates for energy demands
- Resting metabolic rate: Each pound of muscle burns more calories at rest than fat tissue
- Insulin sensitivity: Greater muscle mass correlates with improved cellular response to insulin
When muscle mass declines—through sedentary behavior, aging, or illness—metabolic dysfunction follows predictably. Blood sugar regulation deteriorates. Fat accumulation increases. The cascade effect touches every system.
This explains why resistance training consistently outperforms other interventions for metabolic health in clinical literature. You’re not just building strength; you’re expanding your body’s primary glucose-processing infrastructure.
Myokines: The Hormones Muscles Produce
The myokine discovery represents one of the most significant shifts in exercise science. When muscles contract, they release hundreds of signaling molecules that influence organs throughout the body.
Critical myokines include:
Myokine | Primary Function | Target Organs |
IL-6 | Anti-inflammatory signaling, glucose metabolism | Liver, fat tissue |
Irisin | Fat browning, cognitive protection | Adipose tissue, brain |
BDNF | Neuroprotection, memory formation | Brain, nervous system |
Myonectin | Fatty acid uptake, lipid metabolism | Liver, fat tissue |
The implications extend beyond metabolism. Irisin, for example, crosses the blood-brain barrier and stimulates brain-derived neurotrophic factor (BDNF) production. This creates a direct mechanistic link between muscle activity and cognitive preservation—something observational studies have suggested for years.
Physical activity isn’t merely beneficial because it burns energy. It activates your muscles’ endocrine function, triggering protective cascades that no pharmaceutical currently replicates.
Muscle Loss and Disease Risk: What Research Shows
The relationship between muscle mass and disease outcomes is not subtle. Sarcopenia—the progressive loss of muscle tissue—predicts mortality with uncomfortable precision.
According to data referenced by the Centers for Disease Control and Prevention (CDC), adults lose 3-8% of muscle mass per decade after age 30, accelerating after 60. This loss correlates with:
- Increased falls and fractures
- Higher rates of metabolic syndrome
- Greater hospitalization frequency
- Elevated all-cause mortality
A landmark study in the Journal of the American Medical Association found that low muscle mass predicted surgical complications, cancer survival rates, and recovery from critical illness more reliably than many traditional biomarkers.
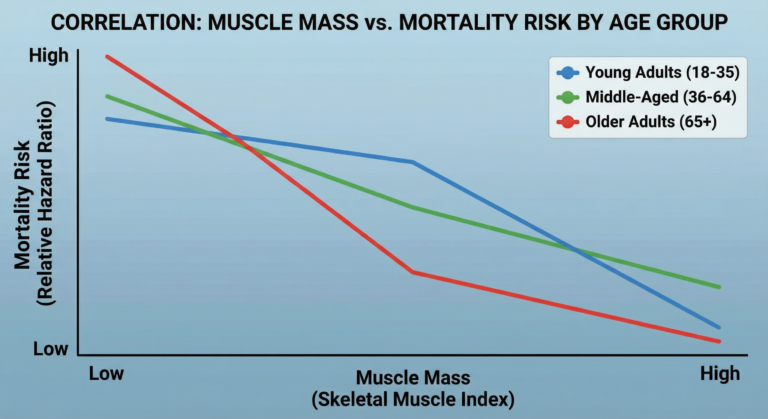
The message is unambiguous: preserving muscle isn’t vanity. It’s survival strategy grounded in outcome data.
Muscles vs. Other Vital Organs: A Comparison
Understanding muscles as a vital organ requires contextualizing their role alongside traditionally recognized organs.
Organ | Primary Functions | Consequences of Dysfunction |
Heart | Blood circulation, oxygen delivery | Cardiovascular disease, mortality |
Liver | Detoxification, protein synthesis, metabolism | Liver failure, metabolic collapse |
Kidneys | Waste filtration, electrolyte balance | Renal failure, toxin accumulation |
Skeletal Muscle | Glucose regulation, hormone secretion, movement, immune modulation | Metabolic disease, frailty, increased mortality |
The comparison reveals something striking: muscle dysfunction produces consequences as severe as those from traditionally prioritized organs. Yet muscle health receives disproportionately less clinical attention.
This disparity matters because muscle is the one vital organ you can actively build. You cannot voluntarily grow your liver or expand your heart. You can, through deliberate intervention, increase your muscle mass and enhance its function at nearly any age.
Myths vs. Facts About Muscle and Health
Persistent misconceptions undermine effective action. Here’s what the evidence actually supports:
Myth 1: Muscles are only important for athletes
Fact: Muscle mass predicts health outcomes across all populations, including sedentary individuals and those with chronic illness. The metabolic and endocrine functions matter regardless of athletic ambition.
Myth 2: Cardio is more important than strength training
Fact: Both modalities offer distinct benefits. However, for metabolic health, glucose regulation, and age-related decline prevention, resistance training produces outcomes cardio alone cannot replicate. Current guidelines from major health organizations recommend both.
Myth 3: Older adults can’t build meaningful muscle
Fact: Research consistently demonstrates muscle protein synthesis remains responsive to resistance training well into the eighth and ninth decades of life. Gains may be slower, but they occur—and they matter clinically.
Myth 4: Protein intake doesn’t significantly affect muscle preservation
Fact: Adequate protein intake (current research suggests 1.2-1.6 grams per kilogram of body weight for active adults) directly supports muscle maintenance and growth. Insufficient protein accelerates age-related muscle loss.
What Experts Say About Muscle as an Organ
Scientific consensus has shifted notably over the past two decades. Leading researchers now explicitly frame muscle tissue as an organ system with systemic responsibilities.
Dr. Bente Klarlund Pedersen, who pioneered myokine research, has published extensively on muscle’s role as “a secretory organ” that communicates with virtually every tissue in the body. Her work, available through PubMed, demonstrates that exercise-induced myokine release mediates many of physical activity’s health benefits.
The World Health Organization’s updated physical activity guidelines explicitly reference the importance of muscle-strengthening activities for all adults, reflecting this evolved understanding. The recommendations aren’t arbitrary—they respond to accumulating evidence about muscle’s metabolic and protective functions.
Clinical researchers studying sarcopenia now advocate for routine muscle mass assessment in healthcare settings, particularly for older adults and those with chronic conditions. The argument: you cannot effectively manage what you do not measure.
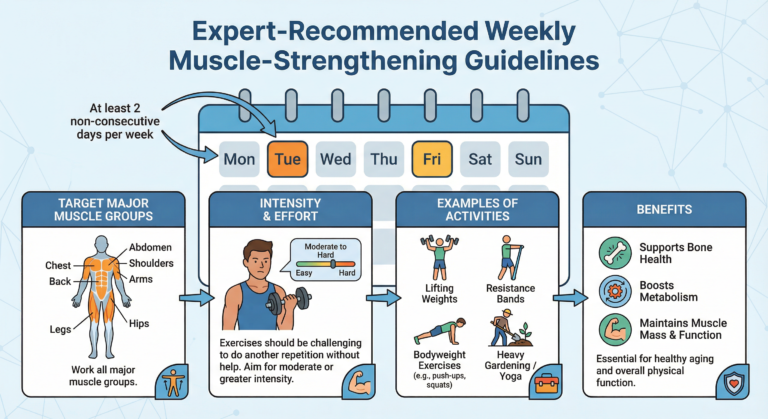
Practical Strategies for Protecting Your Muscle Organ
Understanding muscles as a vital organ demands action, not merely appreciation. Here’s what the evidence supports:
Resistance Training: The Non-Negotiable Foundation
Two to three sessions weekly targeting major muscle groups produces measurable benefits. Progressive overload—gradually increasing resistance—stimulates continued adaptation.
Protein Timing and Quality
Distribute protein intake across meals rather than concentrating it in one sitting. Complete proteins containing all essential amino acids optimize muscle protein synthesis. Leucine, found abundantly in animal proteins and some plant sources, serves as a key trigger.
Address Inactivity Patterns
Prolonged sitting accelerates muscle decline independent of exercise habits. Breaking sedentary periods with brief movement maintains muscle metabolic activity throughout the day.
Prioritize Sleep
Muscle repair and growth occur predominantly during sleep. Chronic sleep deprivation impairs protein synthesis and increases catabolic hormone levels. Seven to nine hours remains the evidence-based target for most adults.
Monitor Trends
Track strength levels over time. Unexplained declines in grip strength or functional capacity warrant investigation. Early intervention prevents accelerated loss.
The Bottom Line: Reframing How You Think About Muscle
The reconceptualization of muscles as a vital organ isn’t semantic gymnastics—it’s a fundamental shift with practical consequences.
When you understand that your muscle tissue secretes hormones, regulates blood sugar, modulates inflammation, protects brain function, and predicts survival outcomes, the motivation equation changes. Resistance training stops being optional enhancement and becomes essential maintenance of a critical organ system.
The choice is yours to make. But the evidence is no longer ambiguous about what that choice means for health outcomes.
External Authoritative References
- Centers for Disease Control and Prevention (CDC) – Physical Activity Guidelines: https://www.cdc.gov/physicalactivity/
- National Institutes of Health (NIH) – Sarcopenia Research: https://www.nih.gov/
